Pulmonary Hypertension | Vibepedia
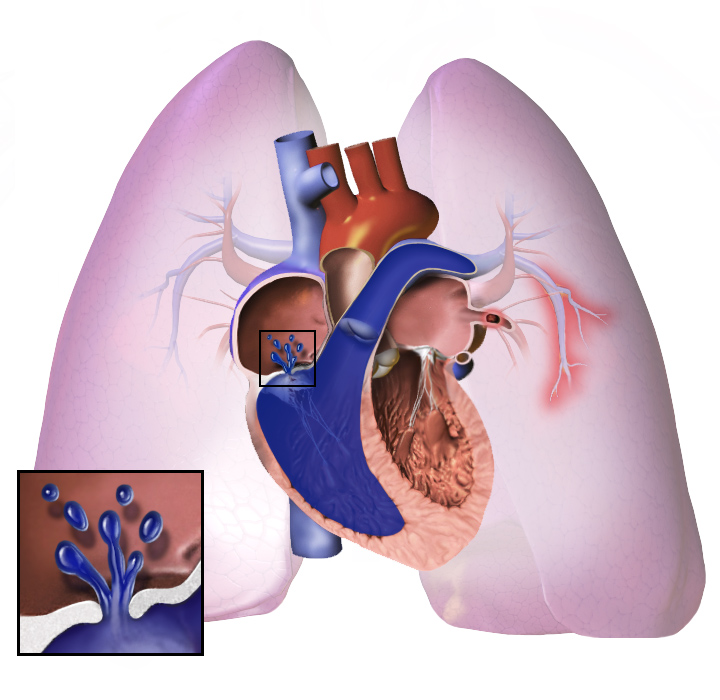
Symptoms like shortness of breath, fatigue, chest pain, and swelling in the legs can be insidious, often mistaken for less serious ailments. Understanding its…
Contents
Overview
The concept of elevated pressure in the pulmonary arteries has a history stretching back to the 19th century, with early observations linking lung congestion to cardiac issues. However, it wasn't until the mid-20th century that pulmonary hypertension began to be recognized as a distinct entity. The classification of PH into distinct groups, a crucial step for targeted treatment, began to solidify in the late 20th century, with major symposia held periodically to refine these categories. The 6th World Symposium on Pulmonary Hypertension in 2018 further refined diagnostic criteria, a change that broadened the diagnostic net and highlighted the progressive nature of the disease.
⚙️ How It Works
Pulmonary hypertension fundamentally involves increased resistance to blood flow through the pulmonary vasculature, the network of arteries and capillaries in the lungs. This resistance, quantified as pulmonary vascular resistance (PVR), can stem from several mechanisms. In pulmonary arterial hypertension (PAH), the most common form, the small pulmonary arteries undergo structural changes: endothelial dysfunction, smooth muscle cell proliferation, and inflammation, leading to narrowing and stiffening of the vessels. This increased resistance forces the right ventricle of the heart to pump against higher pressure, causing it to hypertrophy (thicken) and eventually dilate, leading to right heart failure. Other forms of PH arise from left heart disease, lung diseases like chronic obstructive pulmonary disease (COPD), or chronic blood clots in the lungs (chronic thromboembolic pulmonary hypertension, CTEPH).
📊 Key Facts & Numbers
Key figures in the understanding and treatment of pulmonary hypertension include Dr. Victor Alport, who first described a familial form of the disease. Dr. Stuart Rich at the University of California, Davis, was instrumental in establishing the Pulmonary Hypertension Association (PHA) in 1991, a vital patient advocacy group. Leading research institutions like the Cleveland Clinic, Massachusetts General Hospital, and Johns Hopkins Medicine are at the forefront of clinical trials and research. Pharmaceutical companies such as Actelion (now part of Johnson & Johnson), United Therapeutics, and Bayer AG have developed and marketed critical PAH therapies, including prostacyclin analogs and endothelin receptor antagonists.
👥 Key People & Organizations
Pulmonary hypertension, particularly PAH, has a profound impact on the lives of patients, often leading to significant disability and a reduced quality of life. The chronic shortness of breath and fatigue can limit social engagement and employment opportunities. The disease's rarity and complex symptomatology mean it is often misdiagnosed, leading to delays in treatment and potentially worse outcomes. Patient advocacy groups like the Pulmonary Hypertension Association (PHA) play a crucial role in raising awareness, providing support, and funding research. Cultural portrayals are rare, but the lived experience often involves a constant negotiation with physical limitations and the emotional toll of a serious, chronic illness.
🌍 Cultural Impact & Influence
Current research is intensely focused on developing novel therapeutic targets and improving diagnostic accuracy. The 2018 reclassification by the World Health Organization's Pulmonary Hypertension Scientific Council has spurred new investigations into the underlying mechanisms of each PH group. Advances in imaging, such as cardiac MRI, are enhancing the non-invasive assessment of right ventricular function. Clinical trials are exploring new drug classes, including serotonin transporter inhibitors and soluble guanylate cyclase stimulators, aiming to offer more effective and combination therapies. Though not all patients are surgical candidates, the development of pulmonary thromboendarterectomy (PTE) has been significant for treating CTEPH.
⚡ Current State & Latest Developments
A significant debate revolves around the optimal diagnostic threshold for PH. The shift in diagnostic criteria has led to more patients being diagnosed, raising questions about overdiagnosis and the clinical significance of 'borderline' PH. Another controversy lies in the management of CTEPH, particularly for patients who are not candidates for pulmonary thromboendarterectomy (PTE) or who have persistent PH after surgery. The efficacy and long-term safety of various drug combinations for PAH also remain subjects of ongoing clinical investigation and debate among specialists.
🤔 Controversies & Debates
The future of pulmonary hypertension management points towards more personalized medicine, with treatments tailored to specific PH subtypes and individual patient profiles. Gene therapy and regenerative medicine hold promise for addressing the underlying vascular remodeling. Researchers are also investigating the role of gut microbiome alterations in PH pathogenesis and exploring novel biomarkers for earlier and more accurate diagnosis. The development of less invasive diagnostic techniques and improved risk stratification tools will be crucial for optimizing patient care and potentially achieving long-term remission or even cure for certain forms of PH. The goal is to move beyond merely managing symptoms to directly targeting the disease processes.
🔮 Future Outlook & Predictions
The primary practical application of understanding pulmonary hypertension lies in its diagnosis and management. For physicians, recognizing the subtle symptoms and utilizing diagnostic tools like echocardiography, right heart catheterization, and ventilation-perfusion scans are critical. For patients, adherence to prescribed therapies, including prostacyclin analogs, endothelin receptor antagonists, and phosphodiesterase-5 inhibitors, is paramount. Surgical interventions like pulmonary thromboendarterectomy (PTE) for CTEPH and lung transplantation for severe, refractory PAH are significant applications. Furthermore, the development of specialized PH centers ensures multidisciplinary care, integrating pulmonologists, cardiologists, radiologists, and nurses.
Key Facts
- Category
- science
- Type
- topic